79-year old Jitender Singh recalls the upheavals of being diagnosed with prostate cancer and the gruelling surgery, chemotherapy and follow-ups that spanned over 15 years. Carrying fat folders of his medical records and blood tests to different hospitals. A few years back most of his records were computerized at the hospital he was undergoing check-ups. That was a big change for him as his medical history was now digitalised. However, he plans to move to the south of India to join his son but his medical records though digitalised, cannot travel with him. This EHR vs EMR is exactly why the National Digital Health Mission is launched by the Indian government. EMR is a narrow view while EHR is comprehensive.
Electronic Health Records vs Electronic Medical Records
Electronic medical records (EMRs) is what as a patient you get when you step into any of the large hospitals in your city. Over the past decade, hospitals have shifted their medical record from dusty files in a record room to digital files. No more were physical files to be moved to the physician’s desk, based on prior appointment. Today, digital version of the filed paper charts contains all the medical and treatment history of one patient in one practice. Here is how these EMRs are helpful
Easily identify when a patient is due for a checkup. That’s when you get a call reminding you to fix an appointment.
Doctors can keep a check on their patient’s vital parameters over time such as blood pressure etc.
Use overall patient data within the hospital to improve quality of care offered
That is the limits of EMR. Electronic medical records do not travel. A patient’s record would probably have to be printed or a summary of treatment sent to another specialist outside the hospital environment.
Imagine the impact on Jitender Singh if EMR could travel? Imagine the bigger impact on Jitender’s cancer treatment if AI systems could have flagged early signs of cancer and his medical advisor had a view into the most effect method of treatment based on millions of data points collected from a huge number of patients. That is where EHR makes its need felt.
Also Read: NDHM – Set to Transform India’s Healthcare Through Technology
Electronic Health Records (EHR) will bring together disparate stakeholders right across the healthcare spectrum. Doctors, health service providers, technology solution providers will create and operate systems that will be cloud-based and interoperable so that when a patient comes into the system, irrespective of the point of contact, all his or her data goes into their patient record.
This will be done through different applications that will be developed by different private technology providers but that will all follow certain standardizations that will ensure that applications can communicate with each other. EHR information will move with the patient – to specialists, hospitals, pharmacy, clinical laboratories, the next state or even right across the country.
Data security will be a big part of EHR systems and not all information will be visible. For example, what a specialist sees will not be the same as what the clinic laboratory technician can see of the patient record.
The National Digital Health Mission wants to have every Indian citizen have a unique health ID. The digitised health records will have different identifiers for doctors and different health facilities. This will ensure that only authorized healthcare providers have access to necessary data.
The Health ID will be linked to the NDHM. This centralised health data consent manager will get the patient’s consent for flow of information from the Personal Health Records module.
The NDHM says that it is completely voluntary for each patient to opt for the unique health id. However, just as the Aadhaar id (to which it will be linked) started off as voluntary but became an essential identifier, going forward it is expected that the Health ID will also become a requirement.
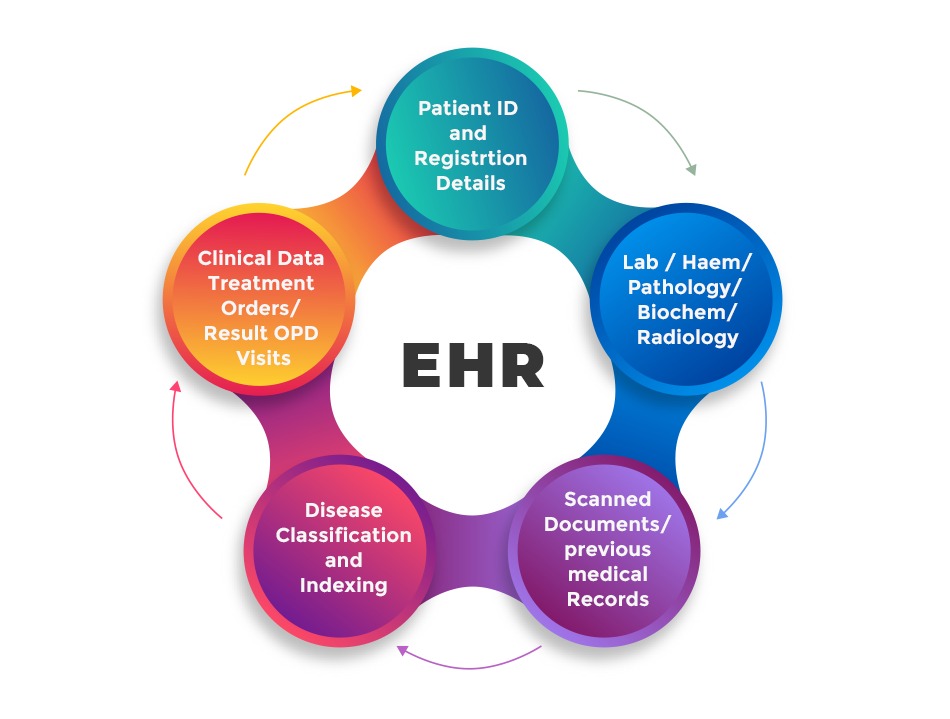
What Information will a Patient’s Electronic Health Record (EHR) contain?
In other countries, EHR is widely implemented. Everyone on the patient’s care team stays informed and can provide decision driven treatment. For the first time, in India, the patient themselves will have access to their information through apps that will be developed to make their information accessible. The data available will be
1.Patient demographics
2.Progress notes
3.Vital signs
4.Medical histories
5.Diagnoses
6.Medications
7.Immunization dates
8.Allergies
9.Radiology images
10.Lab and test results
11.Administrative and billing data
“If we feed in the anonymized data of all public hospitals, we could create a robust decision support system to help newly passed out doctors, this will be a big boost to the accuracy of diagnosis and treatment. We could impact clinical outcomes, predict seasonal outbreaks…”
Prof. Rajendra Pratap Gupta, global public policy expert
Multiple Benefits of EHRs for Patients
There are many reasons why all patients will eventually opt for the unique health ID
- A patient will be able to see his own health records and will be able to see his lab results over time and this will motivate them to keep up with medication and lifestyle changes to improve on the numbers.
- The information available will instantly help in emergency care. For example, life threatening allergies, present medication details etc. can help emergency doctors to adjust treatment
- The physician’s notes will be added on to the patient’s health record in case of hospitalisation and will help in follow-up care, especially when the patient moves to another care setting
- Duplicate testing will be avoided and will help to bring health costs down
- Avoiding any medication errors
- Patient records will help individuals to use remote health services through tele-consultation and e-pharmacy
So yeah, there is more than just a single letter difference between EHR vs EMR. Kerala is the only state that already has implemented EHR of 2.58 crore people in its state government hospitals. Patients can walk into any government hospital without carrying any papers. In fact, this is one of the reasons the state was able to manage the pandemic better than others and train healthcare workers faster and ensure rapid resource mobilization.
Case study: RehabOne – Itech’s Electronic Health Record Software (EHR)
At iTech India, we have an in-depth experience in the health sector and understand the unique challenges involved. We are the trusted technology partners for many American health care providers and can help you get the most out of your EHR solutions.